Book Now Online
Book your next visit today using our online booking platform.
Simply select which clinic you would like to visit and follow the instructions.
Do you suffer from sore feet? Long days got your feet feeling like your walking on hot coals? Been back from your European holiday for a number of weeks and still have ‘holiday feet’? It sounds like you need a trip to the Podiatrist so you can be accurately diagnosed and treated! One particular condition that you could be suffering from is Plantar Fasciitis
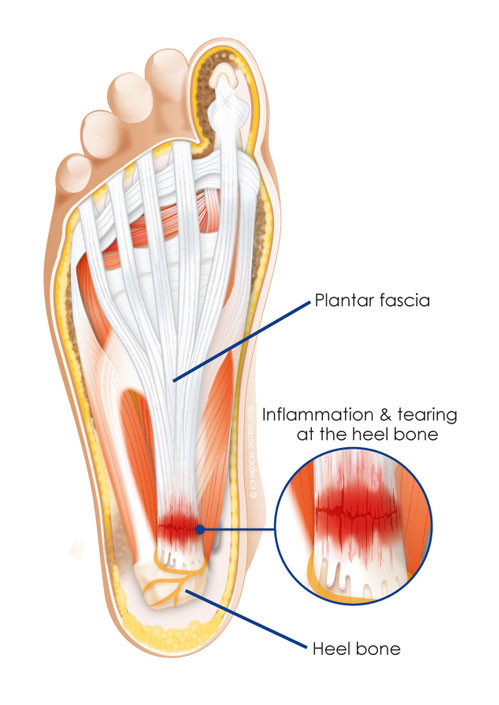
The Plantar Fasciia is a tough piece of connective tissue that lives on the bottom of your foot. It connects the calcaneus (heel bone) to the metatarsals (ball of the foot) and the tip of your toes. Plantar Fasciitis consequently, is the inflammation of that connective tissue. But why does it get inflamed? Before we answer that, we need to establish what the purpose of the connective tissue is.
The plantar fascia (along with other structures) is responsible for your foots arch, which then gives your feet the structural support we need to walk. And we do A LOT of walking…
At 7500 steps a day, we will each walk 216,262,500 steps, which equals around 177,000 kilometers, in our 80-year life time!
That’s not including sports, holidays or any other time that we do more walking than normal. Now if our feet (and bodies) aren’t working properly or in correct biomechanical alignment, you can imagine how that 177,000 kilometres is going to affect our joints, muscles and plantar fascia.
Moving on, plantar fasciitis is the most common foot condition, accounting for up to 15% of foot complaints that require health professional intervention. And again that figure doesn’t include those who don’t seek help, or just think heel pain is normal.
This is where it gets dicey. In most cases Plantar Fasciitis doesn’t have one single causative factor, its multifactorial. As with most injuries to the human body, plantar fasciitis is caused by overusing/overstraining the connective tissue. There are a number of factors that we know influence the straining of the fascia which include, but aren’t limited to;
Of these, poor biomechanics (the study of structure and function of the body) is a particular area of influence on the plantar fascia. Chronically pronated or “flat feet” are a common denominator amongst this demographic. I say chronically because pronation (the flattening of the arch) is a normal and necessary foot function, but when there is an inability to create an arch again the plantar fascia is put under huge tensile (pulling) forces and liable to micro-tearing and rupture.
Poor biomechanics are complicated by the effect of footwear. Flimsy shoes (such as ballet flats or flip flops) and even expensive running shoes may not be suited for your feet. Now, if you add the factor of load (weight gain or increased activity) you get, what I call, the “Trifecta of Foot Pain”.
The chances are you have read this far into this blog because you currently have plantar fasciitis, or have suffered with it in the past. And you would have discovered there are many different modalities for its treatment, but lets briefly talk about a few of the common treatments:
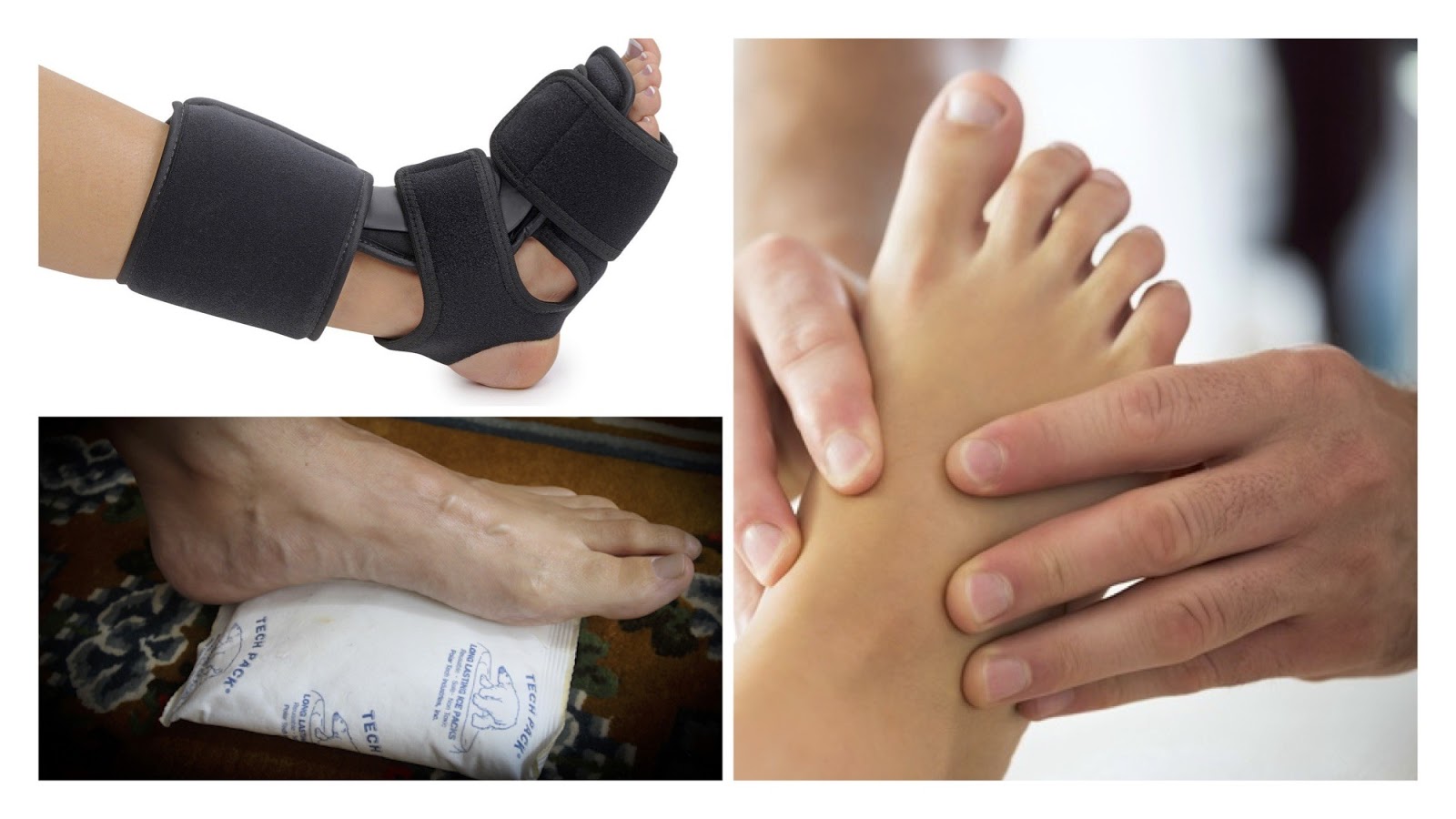
Night splints have been around for two decades for the management of plantar fasciitis. They work on the premise that the problem lies with the plantar fascia being short, and that stretching the ligament will minimise the its chance of tearing when loaded. If your issue is indeed a short plantar fascia you may feel some relief with these splints, but unfortunately they may be short lived as the newly stretched ligament can create feet that are unable to support themselves during loading.
Cryo/Thermotherapy is used for the symptomatic relief of inflamed soft tissue. Cryo (cold) therapy works around the concept of reducing swelling, and Thermo (heat) therapy tries to encourage blood flow, and both have pro’s and con’s. Its important to know that whatever side of the temperature-therapy-spectrum you choose to identify with, both do little to prevent plantar fasciitis from reoccurring long term.
Massage needs no description; sore feet? Massage them! You would be hard-pressed to find anyone who hasn’t felt immediate relief after a massage, and when you combine it with cryotherapy (iced bottle rolling) the immediate effects may be even greater. But again, you are more likely to find yourself on the ‘my-feet-are-still-sore’ side of the fence.
Surgical treatments for plantar fasciitis vary amongst surgeons, and the techniques they use. For this reason I wont talk about any particular procedure, but rather identify that there is typically a significant financial impact (due to periods of non-weight bearing and depending on your job, inability to work), the risk of infection and the risk of reduction of arch integrity by 25%. In saying this, if your in the 10% of the population who does not respond to conservative treatments, surgery is a viable option.
At Podiatry First, we specialise in the treatment of soft tissue injuries, and we are experts in the use of Shockwave Therapy

Extracorporeal Shockwave Therapy (EST) is a highly researched and evidence backed therapy for the treatment of soft tissue and bony injuries. During the treatment, an applicator is applied to the painful area and an acoustic wave carries energy into the affected tissues. This energy interacts with the tissue causing accelerated tissue repair and cell growth, localised analgesia, and mobility restoration; all things that need to be addressed in Plantar Fasciitis!
Your podiatrist should be able to inform you about all the different treatment options for plantar fasciitis, and you should not feel pressured into any treatments you don’t fully understand
So, if you or someone you know is living with foot pain, come drop into Podiatry First. We can identify the causative/contributing factors to your pain, and we can work on them together and establish a rehabilitation program personalised to you.
Thank you for reading!