Medically known as medial tibial stress syndrome is an extremely common repetitive strain injury in runners and running athletes and can be impressively complicated and stubborn.
“Many people are afraid of running because between 30 to 70 percent (depending on how you measure it) of runners get injured every year.”
~ from a fascinating talk about the athletic toughness of human beings, Brains Plus Brawn, by Dr. Daniel Lieberman, evolutionary biologist of “Born to Run” fame
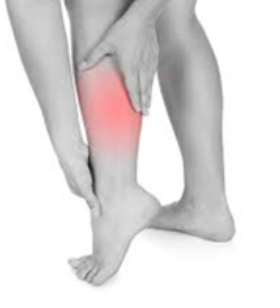
Symptoms
The symptoms of shin splints are:
- Pain and tenderness along the tibia.
- Potential swelling of the lower legs.
- In chronic cases, there may be lumps or bumps felt along the bones.
In severe cases, there may be red patches on the skin around painful areas.
Initially, the pain will stop when exercise stops, but if the condition worsens, the pain can become constant. It is important to have the pain checked by a doctor because other conditions have similar symptoms.
Causes
The exact mechanisms behind shin splints are not fully understood but are thought to involve a variety of different issues.
The causes, however, are relatively clear; shin splints are most commonly associated with repetitive activities that cause stress on the shinbone and the connective tissue that attaches the muscle to the bone.
It is thought that these stresses involve inflammation of the connective tissue that coats the tibia (called the periosteum); this is called periostitis.
Many experts believe that a range of tibial injuries might account for shin splints; some of these could include:
- Tendinopathy: a disease of the tendon.
- Periosteal remodelling: bone growth and regeneration.
- Muscle dysfunction: some muscles may also be involved in shin splints, including:
- Tibialis posterior (inside of the ankle)
- tibialis anterior (running along the shin and top of the foot)
- Soleus (lower calf)
- Overpronation as a cause of shin splints
Foot and ankle overpronation are also thought to be a cause of shin splints. Overpronation of the foot/ankle is when the foot steadily moves downward and toward the centre of the body.
This change in position places more of the arch of the foot in constant contact with the ground. More weight is placed on the inside of the foot (medial) than the outside edge of the foot (lateral).
This abnormal movement causes muscles to fatigue quicker and may place additional stress on the shinbone. In a study investigating shin splints in the British infantry.
“An imbalance in foot pressure with greater pressure on the medial side than on the lateral side was the primary risk factor.”
Diagnosis
Shin splint diagnosis
To diagnose shin splints, your doctor will:
- Perform a physical exam.
- Take your medical history.
- Talk about your activity level.
- Imaging if in doubt ( x-ray)
It is important to rule out other differential diagnosis, such as stress fractures.
Treatment and prevention
Prevention
The following tips might help reduce the chances of shin splints developing:
Lessen impact: consider cross-training with lower impact sports like walking or biking. Choose soft surfaces over hard if possible. Begin any new activities slowly and gradually build up the intensity.
- Wear correct footwear: wearing the right shoes for the job is important. For runners, shoes should be replaced every 300–500 miles.
- Use arch supports (orthotics): these can be helpful, especially for individuals with flat arches.
- Strengthen the area: try toe raises to strengthen the muscles of the lower leg – slowly rise onto tiptoes and back again, repeating ten times.
- Stretch before and after activity
Relative rest, or avoiding the aggravating activity, ice and anti-inflammatory medicines are the mainstay of initial treatment, followed by rehabilitation exercises, such as calf stretching and muscle strengthening. Footwear must be assessed relative to the person’s individual foot type. If the person has foot or gait abnormalities, orthotics may be recommended



